HIL
Healthcare Innovation Lab
The Healthcare Innovation Lab project aimed to develop a business plan for an actual Healthcare Innovation Laboratory to serve as the setting for a public-private partnership on innovation (PPI). The partnership includes businesses, hospitals, knowledge institutions and research institutes, as well as patients and their families in the Capital Region of Denmark.
The potential for systematically developing and testing the simulation process as a user driven method is demonstrated through a number of specific business cases in close collaboration with hospitals, knowledge institutions and the private sector.
Rationale
Can we simulate future hospital, products and processes? Can we accelerate needed experience before we implement a new workflow setting up a branch or develop new telemedicine equipment?
The HIL project brings together health professionals, researchers, business and innovation people’s with the aim to tailor the simulation method for product and process development in healthcare. The project developed innovative prototypes for use on future hospitals, created by the use of simulation in the Capital Region Healthcare Innovation Lab – a Lab, where new solutions can be developed in less time than traditional processes.
Three theme areas will be highlighted in the project:
Project data


- Functional and organizational planning for hospital construction. The focus is on bridging the gap between user and expert solutions in the creation of holistic design of space, organization, technology and performance.
- IT and Telecommunications in clinical practice. Theme area focuses on how ICT and technology can better support patient safety, quality of care, information and communication, thereby contributing to improved efficiency and consistency of patient progress.
- Telemedicine and telemonitoring in the treatment of inpatients and outpatients. Theme area will focus on how technology supported monitoring and information exchange enables both ambulatory and hospitalized patients to handle larger parts of their therapy with support from relevant specialists.
The following description only relates to the telemedicine theme (C), in which In-JeT participated.
Clinical simulation
The telemonitoring scenario was discussed with a view to the needs of the cardiology outpatient clinic at Herlev Hospital and the needs of Bornholms Hospital.
The project started by conducting a series of user centric workshops to elicit basic and functional user demands for new solutions. Various methods adopted from user centric development processes were such as interview, observation, simulation, illustrations, brainstorming, etc.
User situations were explained and evaluated by the project team and daily workflows and clinical procedures were demonstrated.
At several meeting the project team discussed and brainstormed on various aspects of the telemedicine solution in direct interaction with the users (carers, patients, etc.). The aim of the interviews and discussions was to provide the best possible input to the simulations to be performed.
After the initial phase, the project started to analyse the workflow in the cardiac outpatient clinic and to identify possible components that could be substituted by a telemedicine application taking into account that the medical outcome of using telemedicine should better or at least as good as today’s practice.


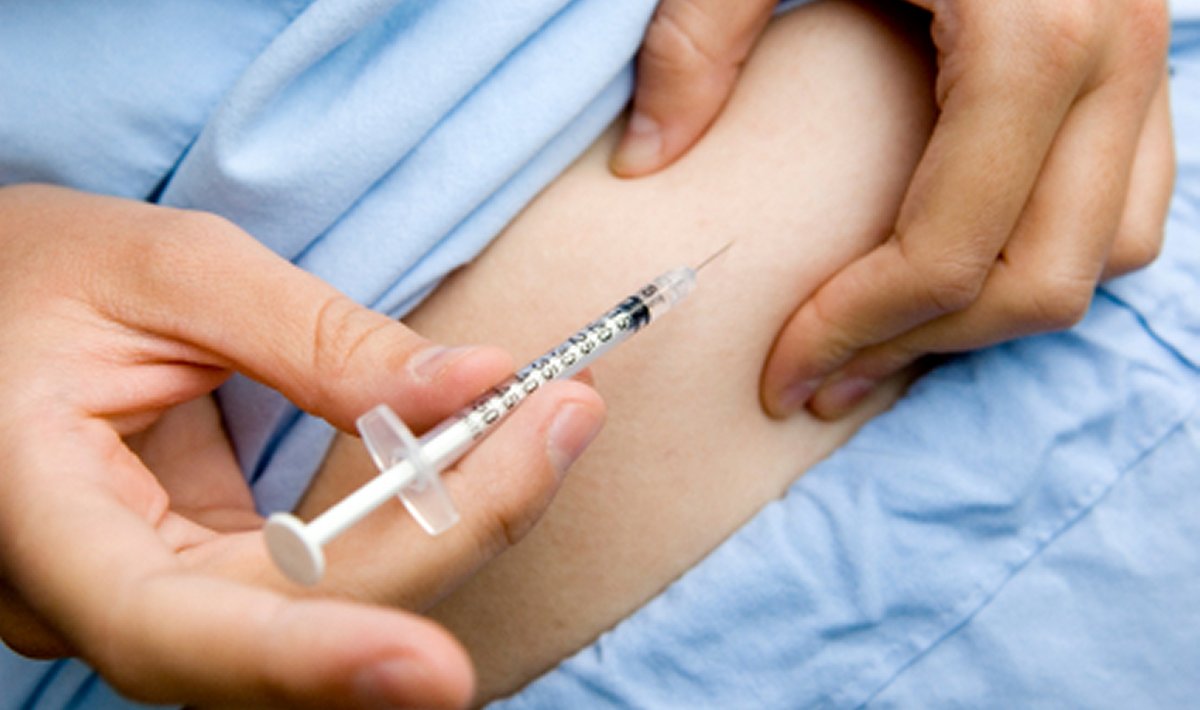
The project focused on the process of up-titration of medication (beta-blockers) for patients with chronic heart failure. Beta-blockers diminish the effects of adrenaline and other stress hormones and reduce the heart rate. The medication is normally initiated in patients with heart failure due to left ventricular systolic dysfunction after other medicine therapy has been completed (diuretic and ACE inhibitor). Beta-blockade therapy for heart failure is introduced in a start low, go slow manner, with assessment of heart rate, blood pressure, and clinical status after each titration.
The up-titration takes 36 weeks and includes 10 visits to the outpatient clinic and typically 8 telephone consultations. The aim of the HIL project is to reduce the number of physical visits to five while increasing the total number of points of contact from 18 to 23. Overall, the telemedicine solution should provide improved care with fewer resources needed by the outpatient staff and better organised workflow in the clinic.
The scenario will be subject to economic modelling and a business case will be developed. As the area to be simulated had been identified, ten use cases were described by the clinicians for simulation with real patients and supporting functionality was developed in a pilot telemonitoring demonstrator. The use cases were:
- The patient measures weight, blood pressure and pulse
- Each measurement is validated by the Patient front end app (separate monitor)
- The clinician reviews the data in tabular and graphical formats
- A simulated weight increase of 1 kg is generated by having the patient carry two water bottles before doing measurement; data validation is repeated.
- The weight increase event is captured by a rule engine and triggers a process to adjust diuretics (medication)
- A notification pops-up at the patient monitor with instructions to adjust diuretics (a separate monitor with patient access to the DiaLog system is used here)
- The simulated weight increase remains after 48 hours even when the patient is taking diuretics
- A new weight increase event is captured and triggers a follow-up action.
- A notification pops up at the patient monitor with instructions to book an e-meeting with the out-patient clinic.
- An e-meeting is conducted using Web Cams and Skype with the aim to have a visual indication on the patient’s physical condition.
Technical and clinical features
The demonstrator is based on DiaLog, a backend health portal provided by IBM, and a patient frontend, providd by In-JeT. The architecture is shown in the Figure below.
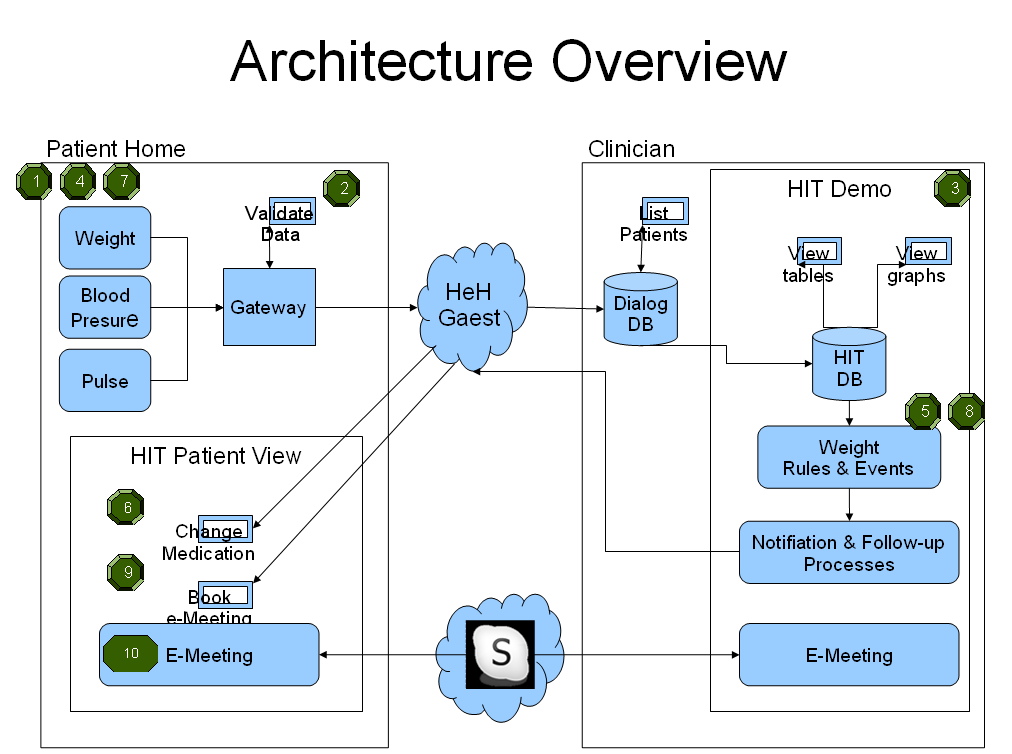
Data are collected from medical devices and transmitted through a home gateway that also acts as patient communication device for validation and video conferencing. Data are send to the DiaLog server where a rules and event engine monitors abnormalities.
The patient logs into the HIL telemedicine application using a touch screen in the home. The user interface is shown in Figure 3. The applications starts by showing a diary for the day with the actual medication that needs to be taken and the physiological parameters that has to be measured. In the HIL project, the patient has to measure blood pressure and weight each morning.
The patient checks-off every time medicine is taken during the day. This allows reminds the patient when to take the medicine and what, and avoids possible double medication. The clinician can monitor the patient’s compliance and assess its impact on the health outcome.
When the patient selects to measure data, a voice instructs him to use the medical device. Data are collected via wireless transmission from the scale or the blood pressure device. When the measurement is completed, the data is displayed on the screen and the patient has to either reject or confirm the values. If confirmed, the data are sent to the DiaLog backend system for review and further analysis by the clinical staff. An acknowledgement is provided to the patient in clear voice.
The DiaLog backend system allows the clinician and the patient (and later on other stakeholders such as the primary care physician, home nurses, etc.) to view and analyse the data in graphical form together with medication, test results and many other relevant data. Each role has its own portal displaying only the information that is relevant and open to the user.

Project Outcomes
The project will create a framework for public-private partnerships (PPP) between companies, hospitals and research institutions in the Capital Region, based on user testing and simulation as user-driven approach. The project aims to deliver concrete results for the participating companies, such as new products, services, processes or strategic partnerships. The goal is to establish a physical and organizational Healthcare Lab, which creates a unique strength of private and public health stakeholders in Denmark by having a professional innovation laboratory used as a source of knowledge and development.
In-JeT’s role in the project
In-JeT provided technological knowhow, prototypes and demonstrators for the telemonitoring part of the project. In-JeT developed a patient front-end based on the LinkSmart® middleware and built the simulation platform for monitoring weight and blood pressure in patients with heart failure during up-titration of their medication.
Partners
Funding
Funded by Erhvervs- og Byggestyrelsen Program for Brugerdreven Innovation.