MovingLife
Mobile eHealth for the VINdication of Global LIFEstyle change and disease management solutions
The MovingLife project was a Support Action (SA) that delivered roadmaps for technological research, implementation practice and policy support with the aim of accelerating the establishment, acceptance and wide use of mobile eHealth solutions that will support lifestyle changes among citizens and improve disease management globally.
The roadmaps addressed a broad group of fundamental issues such as: technology options for applications and services; options for new and improved medical guidelines; user empowerment, acceptance, ethics and privacy; socio-economic environments and policy and regulatory frameworks.
The MovingLife took a global perspective on mHealth not only from the developed world, but equally so from the newly developed and developing regions. Evidence and best practice from use of mHealth solutions in the developing world was taken into account and interviews with experts from newly developed countries such as Brazil and India will be included in the analysis.
Rationale
By now, it is known to most observers that the population in the post-industrial countries is ageing due to falling birth rates and increased life expectancy. At the same time, the number of citizens with chronic conditions associated with ageing and/or unhealthy lifestyles, such as heart and cardiovascular diseases, diabetes, pulmonary diseases and asthma, has reached epidemic proportions.
According to WHO, four of the most prominent chronic diseases – cardiovascular diseases (CVD), cancer, chronic obstructive pulmonary disease and type 2 diabetes – are linked by common and preventable biological risk factors, notably high blood pressure, high blood cholesterol and overweight, and by related major behavioural risk factors: unhealthy diet, physical inactivity and tobacco use.
Project data


Action to prevent these major chronic diseases should focus on controlling these and other key risk factors in a well-integrated manner. Improving chronic patients’ condition and lives will be the major challenge in the future as more and more patients develop chronic and lifestyle related diseases. Studies have consistently shown that when patients are more involved in their own healthcare, they are in many cases able to avoid severe lifestyle related chronic conditions. If they have developed a condition, a more efficient management of their chronic disease with the use of intelligent monitoring will improve patients’ lives and at the same time enable the providers to meet this challenge.
In the European public health sector, there is a growing awareness of the usefulness of eHealth to supporting health systems and services. With the decrease in the labour force over the coming years, there is an even more urgent need to make more eHealth services mobile in order to allow citizens with chronic diseases and disabilities stay longer in the labour markets, reduce the number of lost working days and generally support nomadic working patterns in a global marketplace.
eHealth has thus been on the European Union’s political agenda and among the priorities of the European Commission Information Society policy and research programmes for many years and mHealth is increasingly becoming part of mainstream healthcare priorities as well.
Standing at the crossroads of eHealth, mobile devices and wireless broadband networks, mHealth has found itself in the middle of an explosive growth that these sectors have experienced in the last few years and which is continuing strong, even in the midst of the global recession.
However, it is important to remember that mobile technologies are not objectives, but tools, that should be applied in ways to achieve local, national, and regional health objectives as well as contribute to improving the lives of individuals. For example, mHealth solutions have exceptional potential in addressing important public health challenges such as lifestyle management and chronic disease management.
mHealth
Mobile Healthcare (or mHealth) is a term that refers to the provision of medical services through the use of portable devices with the capability to create, store, retrieve, and transmit data via mobile communications. In technical terms, small devices are used to monitor patient-related data and actively communicate with a central information system; in buildings, communication takes place either over a mobile telephony or fixed line network coupled with WiFi. In open spaces, communication takes place via terrestrial (GSM, GPRS, 3G, 4G, WiMax) communication networks or low-orbit satellite communication.
In recent years, mHealth has emerged as an important sub-segment of the field of electronic health (eHealth). While there is no widely agreed-to definition for these fields, the public health community has coalesced around these working definitions (UNF 2009):
- eHealth: Using information and communication technology (ICT) – such as computers, mobile phones, and satellite communications—for health services and information.
- mHealth: Using mobile communications – such as smart phones, mobile phones or PDA—for health services and information.
eHealth and mHealth are inextricably linked. Both are used to improve health outcomes and their technologies work in conjunction. While there are many stand-alone mHealth programs, it is important to note the opportunity mHealth presents for strengthening broader eHealth initiatives. For example, many eHealth initiatives involve digitizing patient records and creating an electronic backbone that will standardise access to patient data within a national system. A mHealth front-end solution allows patients to continuously access such backend systems, while at the same time being completely mobile. Other mHealth solutions can serve as the access point for entering patient data into national health information systems, and as remote information tools that provide information to healthcare clinics, home providers, and health workers in the field.
Technology Roadmapping
Technology roadmapping has become a widely tool for companies, industries and governmental policy-makers. Yet, in spite of the growing interest in roadmapping and the theoretical and methodological attempts to structure the process, there is not yet a real systematic roadmapping approach or even visioning methodology defined (Codagnone, 2009).
Technology roadmapping is a needs-driven technology planning process to help identify, select, and develop technology alternatives to satisfy a set of product needs. It is a plan that applies to a new product or process, or to an emerging technology. Developing a roadmap has three major uses. It helps reach a consensus about a set of needs and the technologies required to satisfy those needs; it provides a mechanism to help forecast technology developments and it provides a framework to help plan and coordinate technology developments (Garcia, 1999).
The two key products in technology roadmapping are Scenarios (our vision of what may happen) and the Roadmap itself (what needs to be researched/put in place to realise the vision). Of key strategic importance for the roadmap is the State of play, which establishes a baseline for the roadmap and identifies the trends to be used in developing the scenarios. This baseline is used in a Gap Analysis, where it is compared against the scenarios to identify what is lacking in terms of e.g. research in order to make the most desirable aspects of the scenarios to happen and to counter the undesirable ones. On the basis of the gaps thus identified, the key research themes and roadmap charts are developed (Codagnone, 2009). The
MovingLife project will adopt a modified version of technology roadmapping methods in a holistic, policy-oriented approach. We intend to include not only needs for technology research and innovation, but also needs for clinical implementation in disease management and ability to motivate life style changes, needs related to user acceptance, security, safety, and ethics as well as needs for new policy frameworks for e.g. cross-border mHealth and standards.
With a view to the holistic approach and the need to incorporate a range of policy areas in the roadmaps, the project will first develop three thematic roadmaps and identify the different relationships between related areas. The three documents will subsequently be combined in a single document integrating the overall roadmaps for widespread, global use of mHealth solutions.
The three thematic roadmaps aim at clustering related topics contained in the future vision of mHealth as follows:
- Roadmap for technology and application research: addresses technology options for applications and services; wearable devices and BAN/PAN networks; seamless mobile communication and interoperability standards; need for dedicated radio frequency bands for continuous provision of care; security and privacy enhancing technologie, etc.
- Roadmap for clinical and medical uptake: focuses on any need for update of clinical and medical guidelines; new care models; evolution of care spaces; methodology to deliver new knowledge to medical professionals and patients; risk management; patient-doctor relationships, joint and shared care, etc.
- Roadmap for socio-economic and policy frameworks: identifies socio-economic and policy drivers and inhibitors for massive deployment of mHealth related to user acceptance; ethical issues; security, privacy and trust models; cross-border issues; business cases; reimbursement models; mapping of future mHealth applications to the regulatory framework of medical devices; etc.
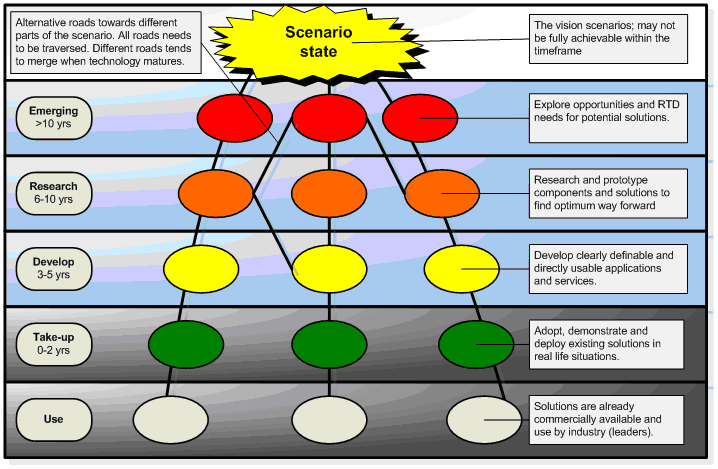
The MovingLife project will use a roadmap notation which illustrates the temporal dimension of the problem with alternative, sequential routes (roads) leading to a future vision of plausible implementation of mHealth solutions. The notation aims at providing a simple overview of issues with high complexity and high uncertainty.
Expected Project Outcomes
The MovingLife roadmaps will pave the way by pointing to a common European understanding and strategy of what is needed to facilitate a massive deployment and take-up of mHealth solutions to citizens. The combined roadmaps will address a range of fundamental issues that are related to the vision of massive deployment and use of mHealth solutions to support lifestyle changes among citizens and improve disease management.
The main expected impact of MovingLife project will be to provide relevant stakeholders, such as policy-makers, industrial actors, healthcare professionals and citizens a comprehensive survey of current resources, needs, guidelines, gaps to be covered, and other relevant information and plans for achieving European leadership in the market and to meet the widespread needs for mobile health solutions.
The roadmaps developed by MovingLife is also expected to have an impact on the direction of future ICT research for sustainable high-quality healthcare, demographic ageing, social and economic inclusion through improved understanding of the technology options. Another impact will be in the development of interoperability standards and secure seamless communication of data. A third impact is to be found in business and regulatory aspects for both private sector-driven and publicly-funded mobile solutions.
References
(Codagnone, 2009) Codagnone, C. (2009). Reconstructing the Whole: Present and Future of Personal Health Systems (preliminary version 16082009). The PHS2020 project funded under FP7.
(Garcia, 1999): Garcia, M.L. and Bray, O.H. (1999). “Fundamentals of Technology Roadmapping”. Strategic Business Development Department, Sandia National Laboratories.
(UNF 2009): Vital Wave Consultation. mHealth for Development (2009). The Opportunity of Mobile Technology for Healthcare in the Developing World. Washington, D.C. and Berkshire, UK: UN Foundation-Vodafone Foundation Partnership.
In-JeT’s role in the project
In-JeT’s role in the MovingLife project was to lead the scenario thinking process and secure that the vision scenarios become realistic, cohesive and comprehensive and provide a solid foundation for development the roadmaps. Moreover, In-JeT worked on state of play, gap analysis and roadmap development in the technology and applications area and the socio-economic area.
Partners
Funding
Co-funded by the European Commission 7th Framework Programme for Research.